Is “Ozempic Rebound” real? We look at the clinical evidence
Introduction
GLP-1 receptor medication such as Ozempic (semaglutide), Semaglutide (semaglutide), and Tirzepatide have transformed the landscape of obesity management and metabolic health. Initially developed for type 2 diabetes, these agents are now widely used to achieve significant weight loss in individuals with obesity or overweight with comorbidities. However, as millions begin and eventually stop these medications, a vital question arises: What happens when the injections stop?
This article explores the phenomenon of weight regain after cessation of weight loss injections (Ozempic, Semaglutide and Tirzepatide), the implications for long-term cardiometabolic health, and emerging strategies to sustain the benefits.
What is Ozempic, Semaglutide and Tirzepatide?
Ozempic and Semaglutide are brand names for semaglutide, a GLP-1 receptor agonist that mimics the hormone glucagon-like peptide-1 to regulate blood glucose, suppress appetite, and slow gastric emptying. While Ozempic is approved for type 2 diabetes, Semaglutide contains a higher dose of semaglutide specifically indicated for weight management.
Tirzepatide, contains tirzepatide, a dual GIP/GLP-1 receptor agonist. It targets both the glucose-dependent insulinotropic polypeptide (GIP) and GLP-1 receptors, offering superior weight loss outcomes compared to semaglutide in clinical trials.


Weight Loss from Ozempic, Semaglutide and Tirzepatide
Clinical trials and real-world data consistently show significant weight loss from treatment with Ozempic, Semaglutide and Tirzepatide:
- Semaglutide: Individuals lost an average of 15% of body weight over 68 weeks (STEP 1 trial).
- Ozempic: While lower in dose, Ozempic still promotes 5–10% body weight reduction in many users (SUSTAIN 1-7 trials)
- Tirzepatide: In the SURMOUNT-1 study of Tirzepatide, participants lost up to 21% of body weight in 72 weeks, positioning it as the most potent weight loss injection to date.
Weight Regain After Stopping Ozempic, Semaglutide and Tirzepatide
Unfortunately, weight regain is a well-documented phenomenon after discontinuation of treatment:
- Weight regain after stopping Semaglutide: In the STEP 1 extension trial, patients from the STEP 1 trial (68 weeks of treatment with semaglutide 2.4mg weekly) were followed up after stopping treatment. Of the original 1961 patients enrolled in the STEP 1 trial, 327 participants were followed up for an additional year. From week 0 to week 68, mean weight loss was 17.3% of body weight with semaglutide 2.4mg per week treatment. Following treatment withdrawal, semaglutide patients regained 11.6 by week 120, resulting in net losses of 5.6% body weight from week 0 to week 120. Cardiometabolic improvements seen from week 0 to week 68 with treatment reverted towards baseline at week 120 for most variables (1).

- Weight regain after stopping Tirzepatide: in the SURMOUNT-4 clinical trial of Tirzepatide, 670 obese or overweight (without diabetes) patients treated with Tirzepatide for 36 weeks lost an average of 20.9% of body weight. At the 36-week mark, they were randomised into placebo and continuing Tirzepatide treatment. From randomisation (at week 36), those switched to placebo experienced a 14% weight regain, and those continuing tirzepatide experienced an additional 5.5% weight reduction during the 52-week double-blind period.
- Real-world evidence mirrors these findings, with many individuals experiencing a rebound in weight and appetite.
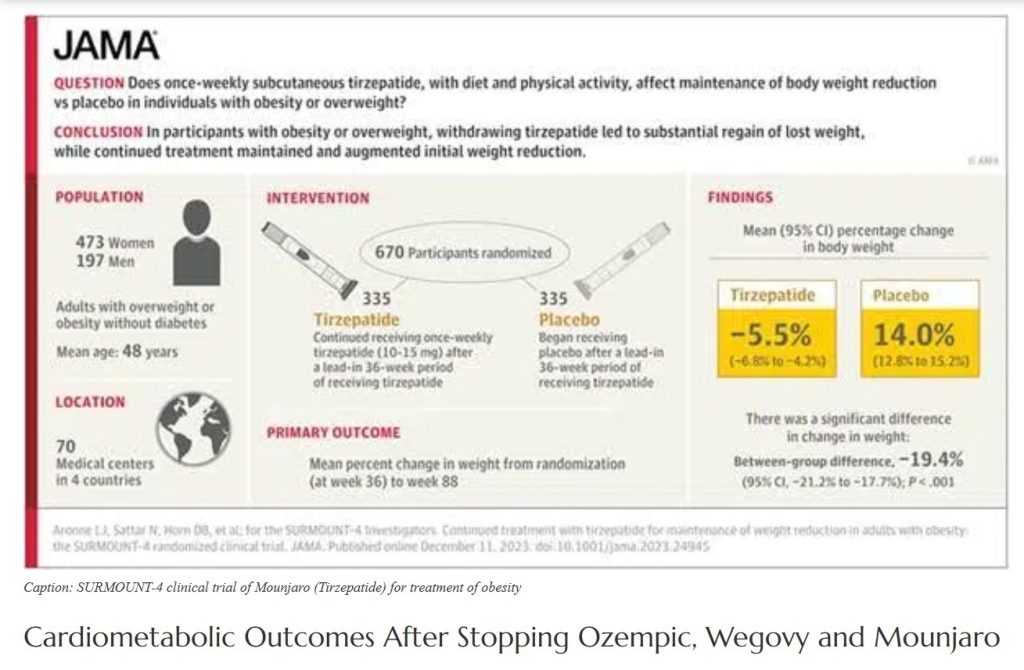
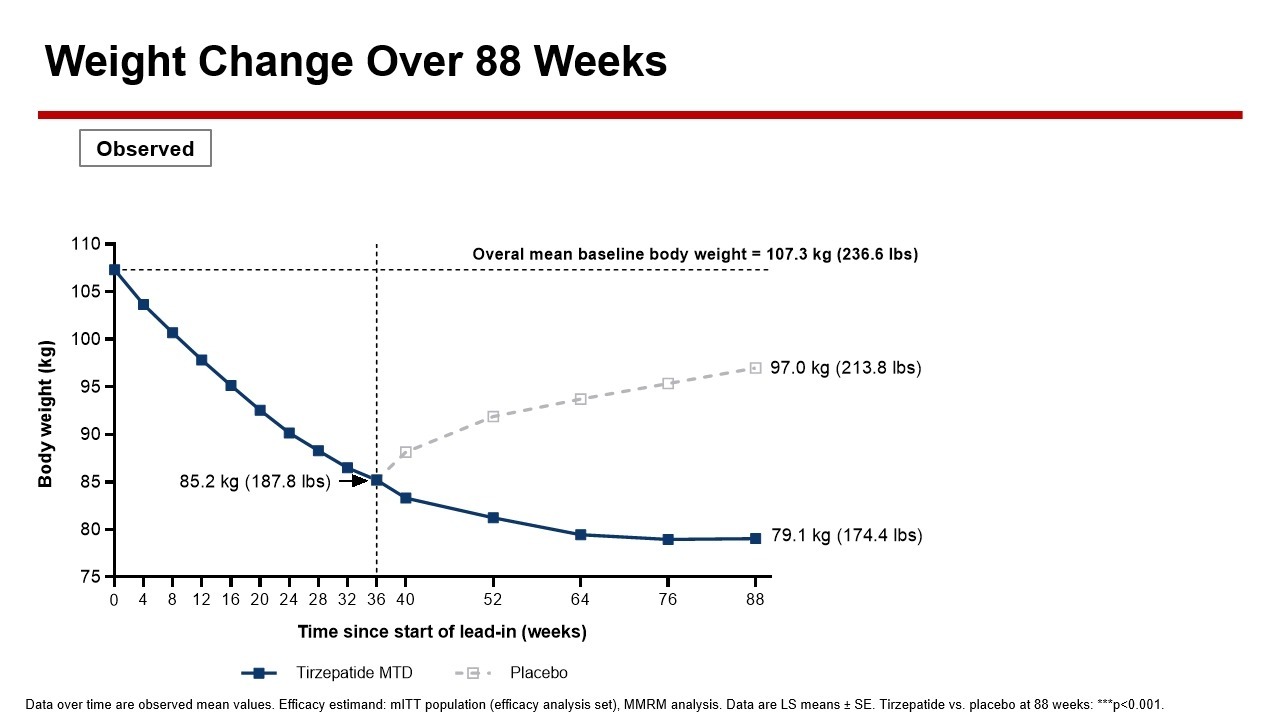
SURMOUNT 4 trial- Weight regain after stopping Tirzepatide after 36 weeks versus continuation of treatment
Cardiometabolic Outcomes After Stopping Ozempic, Semaglutide and Tirzepatide
Beyond weight regain, the discontinuation of GLP-1 agonists may reverse cardiometabolic benefits:
- Blood sugar control often deteriorates, especially in patients with type 2 diabetes.
- Improvements in lipid profiles, blood pressure, and inflammatory markers may wane.
- There is concern that stopping therapy may increase the long-term risk of cardiovascular events, particularly if weight is regained.
Ongoing trials (e.g., SELECT and SURPASS-CVOT) aim to clarify whether continued use is necessary for sustained cardiovascular risk reduction.
Long-Term Strategies to Address Weight Regain
Sustainable weight management requires a multifaceted approach. After an initial ~12-month period of treatment, long-term strategies to maintain a healthy weight include:
- Lifestyle modifications- healthy diet and regular exercise
- Close monitoring of metabolic markers to detect early signs of relapse
- Restarting medication when clinically appropriate
- Long-term low-dose medication, aka “microdose Ozempic”, is an area of active research, with data showing that there may be benefits in weight management and metabolic health.
Personalised treatment plans and regular follow-up are key to preventing rebound weight gain.
Is Microdosing Ozempic the Way Forward?
The concept of “microdosing” Ozempic—using lower, subtherapeutic doses to maintain weight loss—has gained popularity amongst doctors and patients. This is still an area of active research. Reasons where microdosing Ozempic may be appropriate include:
1) Tapering off from standard treatment dosages- Microdose Ozempic as maintenance treatment
This is probably the most common reason why a patient would microdose Ozempic- to maintain the results from Ozempic treatment after coming off a ~6-12 month treatment course.
2) Gradual weight loss
Patients who wish to achieve their weight loss goals more gradually, over a longer time period, may consider microdose Ozempic
3) Fewer side effects
Patients who are experiencing significant side effects from Ozempic at treatment doses may benefit from low-dose Ozempic
4) Lower risk of Ozempic Face
Ozempic Facedevelops due to excessive and rapid weight loss. Gradual weight loss reduces the chance of developing Ozempic Face
5) Affordability
Patients who are able to experience good effects at lower Ozempic doses may prefer to microdose Ozempic to save costs.
Conclusion
Ozempic, Semaglutide, and Tirzepatide represent effective tools in the fight against obesity and metabolic disease. Yet, weight regain after treatment discontinuation is common and may undermine the long-term benefits unless proactively managed.
Sustained success requires lifelong commitment to metabolic health—through continued pharmacotherapy and lifestyle changes. As the field evolves, more data will clarify the optimal treatment duration, dosing to ensure lasting results.
References
- Wilding et al. STEP 1 Study Group. Weight regain and cardiometabolic effects after withdrawal of semaglutide: The STEP 1 trial extension. Diabetes Obes Metab. 2022 Aug;24(8)
- Aronne et al. SURMOUNT-4 Investigators. Continued Treatment With Tirzepatide for Maintenance of Weight Reduction in Adults With Obesity: The SURMOUNT-4 Randomised Clinical Trial. JAMA. 2024 Jan 2